Before you get snipped, know the facts.
If you are done raising children and have decided that you’d like to get permanent modifications on your reproduction, vasectomy is a highly favorite technique.
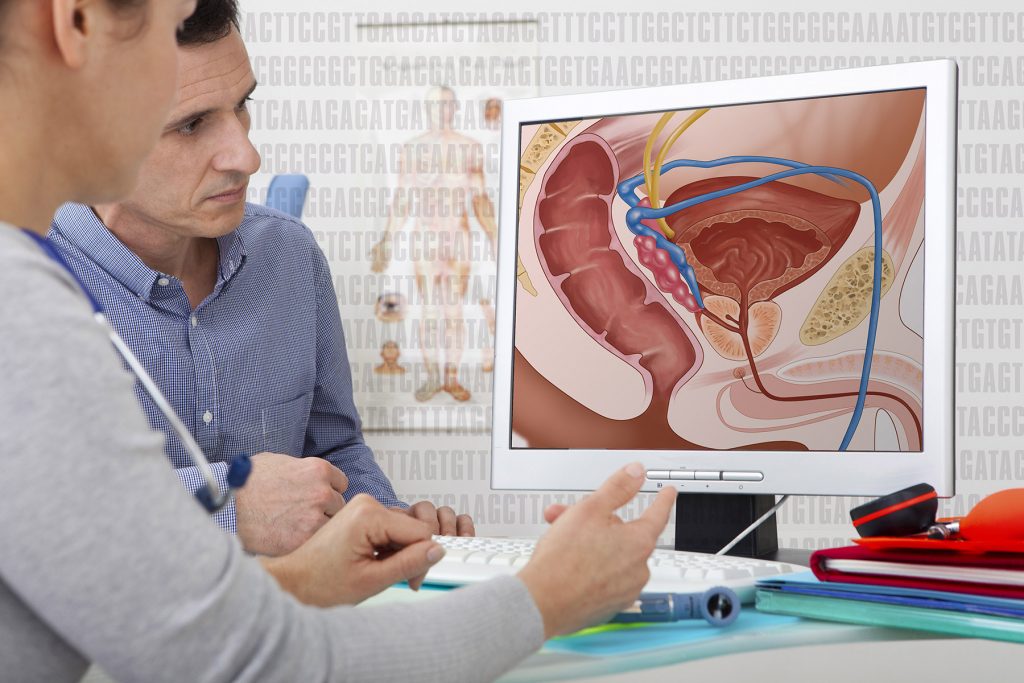
Defining Vasectomy
Also known as male sterilization, vasectomy is a surgical procedure preventing sperm release, which makes this one of the most effective methods of pregnancy prevention. The process usually takes place either inside a clinic or a hospital.
Vasectomy has two types: the no-scalpel method and the incision method. Between the two, the no-cut way is more recommended since it lowers the risk of complications and infection and accounts to lesser heal time.
“Many gynecologists have training in the art of vasectomy. Vasectomy is a safe and cost-effective method of contraception,” writes Mark Borigini, M.D.
Permanence
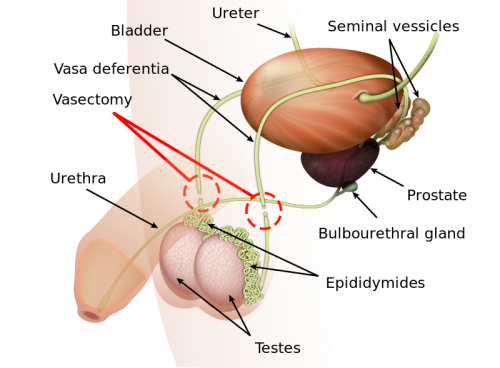
Technically, what happens in a vasectomy procedure is that the vas deferens, the two tubes that serve as sperm passages, are cut or blocked, preventing sperm from mixing with semen. The undelivered sperms will stay inside the testicles for absorption by the body in approximately three months. After the procedure, you will still produce the same amount of semen but will no longer contain sperms so you will not cause impregnation. Just in case this is news to you, the sperms get you pregnant and not the semen.
“While many men will be happy to use contraception that is easily reversible and does not mess up their sex drive or make them feel strange, we don’t yet know how many men would use it regularly, or how many women would trust that their male partners were actually using it,” writes Paul Joannides, Psy.D.
So, as a recap, vasectomy is:
- Permanent, therefore, you can no longer reproduce.
- One of the most effective ways of family planning.
- Stops the sperms, not the semen.
- Not a cancellation of ejaculation or orgasm.
- More preferred than tubal ligation since it is way quicker, cheaper, and safer.
Initial Call for Concern
The first report for vasectomies was in the late 1980s where scientists insisted on the emergence of developing prostate cancer due to vasectomies. Over the years, there have been studies materializing in an attempt to establish the misleading plausibility that that two may somehow be related.
Until now, there have been contrasting ideas and theories as to how one connects with the others but the majority of the opposing side, the ones who believe that the two are correlated, are usually rebutted by entirely convincing studies. Some research is straightforward in corroborating the weak association of prostate cancer and vasectomies, saying the robust investigation and study design were increasingly close to null.
Prostate Cancer after Vasectomies
Currently, there is no substantial evidence of an increased risk of having prostate cancer after vasectomies. Though there have been controversies revolving around the procedure about it being a long-term risk to develop prostate cancer, studies are stating that researchers did not discover any sign of elevated risk especially regarding the more advanced stage of the disease. Apart from that, the study also emphasized that deaths in men are not connected to vasectomy-related prostate cancer.
Researchers conclude that studies contradicting vasectomy’s relation to being prone to prostate cancer are piling up, strengthening the initial investigations and findings. Therefore, there is very little reason to be alarmed that vasectomies are likely to cause prostate cancer.
In Conclusion
If you’re really up for it, do it. Do not let fears and false stories cloud the decision you are doing for the future of your family. Though there are tons of causes for the occurrence of prostate cancer, vasectomy is not one of them. The bottom line is, vasectomies are safe because science said so. Now, go forth and control the population!
“If we succeed, there may be a glimmer of hope of mitigating our own ecological overshoot, and the potential Malthusian nightmares of the future,” writes Michael Mills, Ph.D.
